The Spanish Flu
The 1918 influenza pandemic (January 1918 – December 1920; colloquially known as Spanish flu)
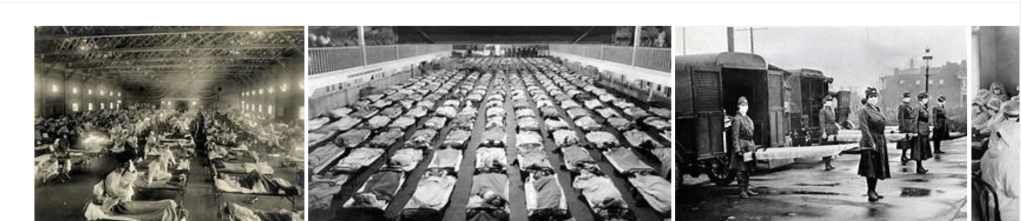
The 1918 influenza pandemic (January 1918 – December 1920; colloquially known as Spanish flu) was an unusually deadly influenza pandemic, the first of the two pandemics involving H1N1 influenza virus, with the second being the swine flu in 2009. It infected 500 million people around the world, or about 27% of the then world population of about 1.8 billion, including people on remote Pacific islands and in the Arctic. The death toll is estimated to have been 50 million, and possibly as high as 100 million (about 3 to 6 percent of Earth’s population at the time), making it one of the deadliest epidemics in human history. Historical and epidemiological data are inadequate to identify with certainty the pandemic’s geographic origin.
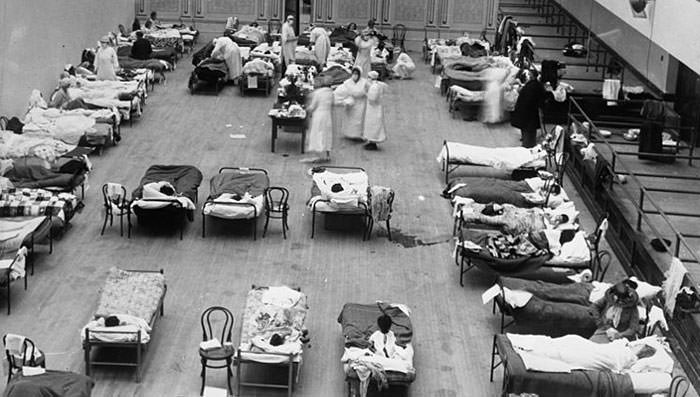
Infectious diseases already limited life expectancy in the early 20th century, but life expectancy in the United States dropped by about 12 years in the first year of the pandemic. Most influenza outbreaks disproportionately kill the very young and the very old, with a higher survival rate for those in-between. However, the Spanish flu pandemic resulted in a higher than expected mortality rate for young adults.

To maintain morale, wartime censors minimized early reports of illness and mortality in Germany, the United Kingdom, France, and the United States. Papers were free to report the epidemic’s effects in neutral Spain (such as the grave illness of King Alfonso XIII). These stories created a false impression of Spain as especially hard hit,[13] thereby giving rise to the pandemic’s nickname, “Spanish flu”.
Scientists offer several possible explanations for the high mortality rate of the 1918 influenza pandemic. Some analyses have shown the virus to be particularly deadly because it triggers a cytokine storm, which ravages the stronger immune system of young adults. In contrast, a 2007 analysis of medical journals from the period of the pandemic found that the viral infection was no more aggressive than previous influenza strains. Instead, malnourishment, overcrowded medical camps and hospitals, and poor hygiene promoted bacterial superinfection. This superinfection killed most of the victims, typically after a somewhat prolonged death bed
1918 Spanish Flu historical documentary
History
Hypotheses about the source
The major troop staging and hospital camp in Étaples, France, was identified by researchers as being at the center of the Spanish flu. The research was published in 1999 by a British team, led by virologist John Oxford.[20] In late 1917, military pathologists reported the onset of a new disease with high mortality that they later recognized as the flu. The overcrowded camp and hospital was an ideal site for the spreading of a respiratory virus.
The hospital treated thousands of victims of chemical attacks, and other casualties of war. 100,000 soldiers were in transit through the camp every day. It also was home to a live piggery, and poultry was regularly brought in for food supplies from surrounding villages. Oxford and his team postulated that a significant precursor virus, harbored in birds, mutated and then migrated to pigs kept near the front.
There have been claims that the epidemic originated in the United States. Historian Alfred W. Crosby claimed that the flu originated in Kansas, and popular author John Barry described Haskell County, Kansas, as the point of origin. It has also been claimed that, by late 1917, there had already been a first wave of the epidemic in at least 14 US military camps.
One of the few regions of the world that were seemingly less affected by the 1918 flu pandemic was China, where there may have been a comparatively mild flu season in 1918 (although this is disputed, see #Less-affected areas). There were relatively few deaths from the flu in China compared to other regions of the world. This has led to speculation that the 1918 flu pandemic originated from the country of China itself.
The relatively mild flu season and lower rates of flu mortality in China in 1918 may be explained due to the fact that the Chinese population had already possessed acquired immunity to the flu virus. Thus in 1918, China was spared from the worst ravages of the pandemic, due to the apparent greater resistance to the virus among the Chinese population compared to other regions of the world
Earlier hypotheses put forward varying points of origin for the epidemic. Some hypothesized that the flu originated in East Asia, a common area for transmission of disease from animals to humans because of dense living conditions. In 1993, Claude Hannoun, the leading expert on the 1918 flu for the Pasteur Institute, asserted the former virus was likely to have come from China. It then mutated in the United States near Boston and from there spread to Brest, France, Europe’s battlefields, Europe, and the world with Allied soldiers and sailors as the main disseminators.
He considered several other hypotheses of origin, such as Spain, Kansas and Brest, as being possible, but not likely.
Political scientist Andrew Price-Smith published data from the Austrian archives suggesting the influenza had earlier origins, beginning in Austria in early 1917.
In 2014, historian Mark Humphries argued that the mobilization of 96,000 Chinese laborers to work behind the British and French lines might have been the source of the pandemic. Humphries, of the Memorial University of Newfoundland in St. John’s, based his conclusions on newly unearthed records. He found archival evidence that a respiratory illness that struck northern China in November 1917 was identified a year later by Chinese health officials as identical to the Spanish flu.
A report published in 2016 in the Journal of the Chinese Medical Association found no evidence that the 1918 virus was imported to Europe via Chinese and Southeast Asian soldiers and workers. It found evidence that the virus had been circulating in the European armies for months and possibly years before the 1918 pandemic.
Spread

When an infected person sneezes or coughs, more than half a million virus particles can spread to those nearby. The close quarters and massive troop movements of World War I hastened the pandemic, and probably both increased transmission and augmented mutation. The war may also have increased the lethality of the virus. Some speculate the soldiers’ immune systems were weakened by malnourishment, as well as the stresses of combat and chemical attacks, increasing their susceptibility.
A large factor in the worldwide occurrence of this flu was increased travel. Modern transportation systems made it easier for soldiers, sailors, and civilian travelers to spread the disease.
In the United States, the disease was first observed in Haskell County, Kansas, in January 1918, prompting local doctor Loring Miner to warn the U.S. Public Health Service‘s academic journal. On 4 March 1918, company cook Albert Gitchell, from Haskell County, reported sick at Fort Riley, an American military facility that at the time was training American troops during World War I, making him the first recorded victim of the flu. Within days, 522 men at the camp had reported sick.
By 11 March 1918, the virus had reached Queens, New York. Failure to take preventive measures in March/April was later criticised.
In August 1918, a more virulent strain appeared simultaneously in Brest, France; in Freetown, Sierra Leone; and in the U.S. in Boston, Massachusetts. The Spanish flu also spread through Ireland, carried there by returning Irish soldiers. The Allies of World War I came to call it the Spanish flu, primarily because the pandemic received greater press attention after it moved from France to Spain in November 1918. Spain was not involved in the war and had not imposed wartime censorship.
Mortality
“In terms of single events causing major loss of life, it surpassed the First World War (17 million dead), the Second World War (60 million dead), and possibly both put together. It was the greatest tidal wave of death since the Black Death, perhaps in the whole of human history.” Laura Spinney, Pale Rider: The Spanish Flu of 1918 and How It Changed the World
Coronavirus
A coronavirus is one of a number of viruses that cause diseases in mammals and birds. In humans, the viruses cause respiratory infections, including the common cold, which are typically mild, though rarer forms such as SARS, MERS and 2019-nCoV can be lethal. Symptoms vary in other species: in chickens, they cause an upper respiratory disease, while in cows and pigs coronaviruses cause diarrhea. There are no vaccines or antiviral drugs to prevent or treat human coronavirus infections.
Coronaviruses are in the subfamily Orthocoronavirinae in the family Coronaviridae, in the order Nidovirales. They are enveloped viruses with a positive-sense single-stranded RNA genome and a nucleocapsid of helical symmetry. The genome size of coronaviruses ranges from approximately 26 to 32 kilobases, the largest for an RNA virus.
The name “coronavirus” is derived from the Latin corona, meaning crown or halo, which refers to the characteristic appearance of the virus particles (virions): they have a fringe reminiscent of a crown or of a solar corona.
Coronavirus fake news infects the media
See: Wikipedia Coronavirus for more details
Black Death
The Black Death, also known as the Pestilence (Pest for short), the Great Plague or the Plague, or less commonly the Black Plague, was one of the most devastating pandemics in human history, resulting in the deaths of an estimated 75 to 200 million people in Eurasia, peaking in Europe from 1347 to 1351.[1][2][3] The bacterium Yersinia pestis, which results in several forms of plague (septicemic, pneumonic and, the most common, bubonic) is believed to have been the cause.[4] The Black Death was the first major European outbreak of plague and the second plague pandemic.[5] The plague created a number of religious, social and economic upheavals, with profound effects on the course of European history.
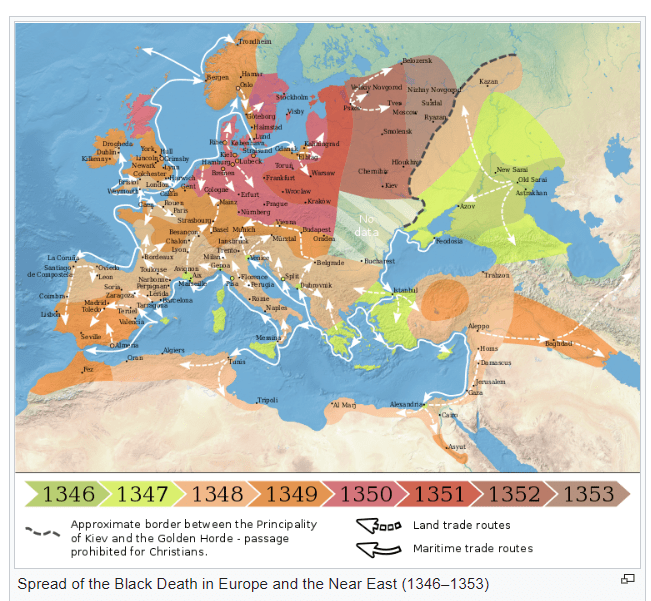
The Black Death is thought to have originated in the dry plains of Central Asia or East Asia, where it travelled along the Silk Road, reaching Crimea by 1343. From there, it was most likely carried by fleas living on the black rats that traveled on all merchant ships, spreading throughout the Mediterranean Basin and Europe.
The Black Death is estimated to have killed 30% to 60% of Europe’s population. In total, the plague may have reduced the world population from an estimated 475 million to 350–375 million in the 14th century. It took 200 years for the world population to recover to its previous level. The plague recurred as outbreaks in Europe until the 19th century.
BBC Documentary THE BLACK DEATH
Chronology
Origins of the disease
Main article: Black Death migration
The plague disease, caused by Yersinia pestis, is enzootic (commonly present) in populations of fleas carried by ground rodents, including marmots, in various areas, including Central Asia, Kurdistan, Western Asia, North India, and Uganda. Due to climate change in Asia, rodents began to flee the dried-out grasslands to more populated areas, spreading the disease. Nestorian graves dating to 1338–1339 near Issyk-Kul in Kyrgyzstan have inscriptions referring to plague and are thought by many epidemiologists to mark the outbreak of the epidemic, from which it could easily have spread to China and India. In October 2010, medical geneticists suggested that all three of the great waves of the plague originated in China.
The 13th-century Mongol conquest of China caused a decline in farming and trading. Economic recovery had been observed at the beginning of the fourteenth century. In the 1330s, many natural disasters and plagues led to widespread famine, starting in 1331, with a deadly plague arriving soon after. Epidemics that may have included the plague killed an estimated 25 million Chinese and other Asians during the fifteen years before it reached Constantinople in 1347.
The disease may have travelled along the Silk Road with Mongol armies and traders or it could have arrived via ship. By the end of 1346, reports of plague had reached the seaports of Europe: “India was depopulated, Tartary, Mesopotamia, Syria, Armenia were covered with dead bodies”.
Plague was reportedly first introduced to Europe via Genoese traders from the port city of Kaffa in the Crimea in 1347. During a protracted siege of the city by the Mongol army under Jani Beg, whose army was suffering from the disease, the army catapulted infected corpses over the city walls of Kaffa to infect the inhabitants. The Genoese traders fled, taking the plague by ship into Sicily and the south of Europe, whence it spread north.[20] Whether or not this hypothesis is accurate, it is clear that several existing conditions such as war, famine, and weather contributed to the severity of the Black Death. Among many other culprits of plague contagiousness malnutrition even if distantly also had an effect as a contributor to such an immense loss in European population since it lead to weakened immune systems.
5 Diseases That Could Kill You In 24 Hours
Youngster gets E.coli after park lake swim
Here’s a story about my son Jude, now 12 who contacted E Coli from local river.

A Leyland youngster who enjoyed a paddle in the water at a beauty spot ended up being struck down with the E.coli bug.
Jude Chambers, four, of Great Park Drive, went to Cuerden Valley Park with his parents Steve and Simone three weeks ago.
Mum Simone, 39, who also has a daughter Autumn, said: “Jude had been paddling in the stream on both the Friday and the Saturday and on the Monday, he began complaining of stomach cramps and vomiting.
“A couple of days later, he began suffering from diarrhoea which kept getting worse and became uncontrollable.”
When Jude’s condition worsened, his parents took a sample to the doctor for testing and the following day, they received a telephone call telling them Jude had E.Coli and to take him to Royal Preston Hospital.
Simone, who is a ballet and contempary dancer and teacher, said: “When you first hear the word E-coli, you start thinking really horrible things and we were really upset and worried about Jude.
“Royal Preston Hospital carried out tests to check Jude’s kidneys and liver were affected. Luckily, they weren’t and we were allowed to take him home.
“He carried on suffering from the diarrhoea for a week and he is now a lot better, although he gets very tired and still gets stomach pains.
“However, we have sent three samples for testing and he is still testing positive for E.coli three weeks on.
“Health protection experts came to our home and after hearing that Jude had been paddling in the water, they suspect he got the E.Coli from the water.”
Jude is a pupil at Lever House Primary School in Leyland, but has not been to school since becoming ill.

